
-
Anti-Aging Skincare: Ingredients and Techniques for Youthful Skin
posted: Apr. 15, 2024.

-
Mole Check: Importance of Regular Skin Exams for Early Detection
posted: Apr. 02, 2024.

-
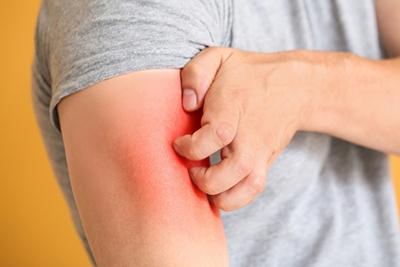
Are You Dealing with a Rash?
posted: Mar. 07, 2024.
-
What You Need To Know About Cosmetic Dermatology
posted: Mar. 01, 2024.

-
Skin Rash Treatment
posted: Feb. 07, 2024.

-
Cosmetic Dermatology: Exploring Non-Surgical Aesthetic Procedures
posted: Feb. 01, 2024.

-
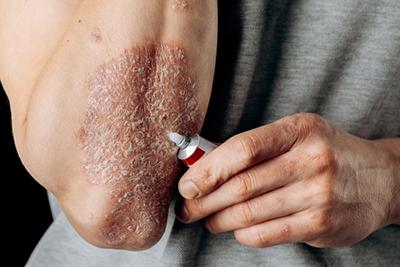
Eczema and Psoriasis: Understanding and Managing Chronic Skin Conditions
posted: Jan. 09, 2024.
-
Common Skin Conditions
posted: Jan. 01, 2024.

-
Best Ways To Protect Your Skin
posted: Dec. 07, 2023.

-
Managing Chronic Skin Conditions
posted: Dec. 01, 2023.
-
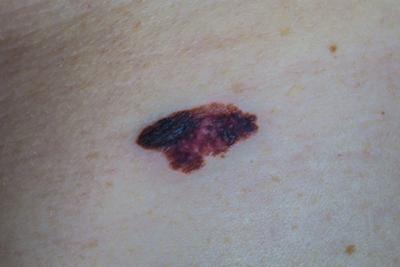
FAQs About Melanoma
posted: Nov. 06, 2023.
-
Rosacea: Understanding Triggers and Effective Treatment Approaches
posted: Nov. 01, 2023.

-
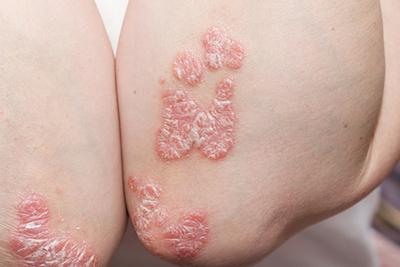
Suffering From Psoriasis?
posted: Oct. 06, 2023.
-
What Can a Chemical Peel Do for Your Skin?
posted: Oct. 01, 2023.

-
Acne Treatment Options
posted: Sep. 11, 2023.

-
Why Taking Care of Your Skin Is Important
posted: Sep. 01, 2023.

Our Location
Office Hours
Monday:
7:30 am-4:00 pm
Tuesday:
7:30 am-4:00 pm
Wednesday:
7:30 am-4:00 pm
Thursday:
7:30 am-4:00 pm
Friday:
7:30 am-4:00 pm
Saturday:
Closed
Sunday:
Closed
